Deshae Lott
determined sojourner
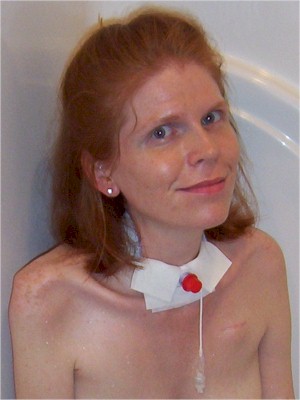
FAQ: Personal care issues
Can you spend time out of the wheelchair?
Yes, I do in order to travel beyond the home and when I lay in bed and use the restroom. This involves someone, almost always my husband, leaning over me, squatting, and putting his arms around me, locking his elbows in place tightly against my ribs, and picking me up. However, particularly strong guys can pick me up and set me down like a baby. It is to our great benefit that my weight seldom goes higher than 105 pounds. I also have a Hoyer lift that others can use for taking me to the bathroom, but it means I must sit on a harness with a cut-out in the bottom. Also, I have a Multirall lift/track system stretching from our bed past the shower and tub and to the toilet that I can use, although also that would mean using a sling and a strap next to it to carry the vent hung from it. Unfortunately, I'm now to the point where for any of these operations, I only can be off the vent for a couple of minutes at most. So, during hair washing, sitting on a toilet, and taking a bath I have to get hooked back up to it.
How do you use the bathroom?
Fortunately, except when I was unconscious, I do so without a catheter -- a potential source of infection. There are three possibilities regarding urination (from the perspective of a female, obviously), not counting using the lift/track system (which is much like manually being lifted and placed on the toilet).
One, my husband transfers me to the toilet at intervals throughout each day. My toileting routine dictates my clothing choices to some degree. Although I don't have any specialty clothing for wheelchair users, we find it easier to manage restroom trips when I wear certain styles of clothing. For example, I wear many wrap skirts or short shirts now; the best skirts are neither tight nor clingy in fabric; they must fall easily. My husband finds it strains his back less, if no one is around to assist him, when he’s holding me and maneuvering my panties if I wear smaller styles of those as well: a thong or g-string is easiest up and down for him.
Two, in my standing wheelchair I am able to use a female urinal that has a removable cup that, when placed correctly, extends from the perineum in back to my lower abdomen in front. I get the chair to stand me up, not all of the way but perhaps at a 75-degree angle, have my skirt lifted and underwear (if wearing any) pulled down in front (again, a g-string or thong pose little difficulty for this task), have the detachable cup put between my legs with a tight seal, and the remainder of the urinal attached extending out. Then the urinal can be supported up against me from the bottom. After finishing, the whole thing is slid out. Obviously, this works only for urination. Having a wheelchair with a wide footplate is necessary for me to spread my legs enough before standing for this to work. Also, I have found that urinating at frequent intervals seems to help, as I suspect when standing if my bladder is too full it distends in a way when I stand that makes it difficult to start urinating.
Three, an alternative way for urinating later at night or earlier in the morning or whenever I'm in bed is to use a different female urinal that is flatter in profile. To succeed without leaks took us a little practice, but really it’s a matter of spreading my legs out of the way like a frog's and pressing the longest-protruding lip of the urinal firmly against my perineum which means the remainder does not have to press around and encompass the area surrounding my urethra unlike when standing. Again, this method accounts only for urination. Note, the female urinals I use are adaptations to a bed pan and not like the urinals affixed to walls in men’s public restrooms. Also, best results are obtained by having pubic hair removed from around the urethra.
Before vent life, using grab bars I could be propped standing, legs spread somewhat and rams out holding the bars, and lock my legs into place where then somebody could gently pull up or down my underwear before grabbing me on the way to seating me somewhere. Regrettably, that's no long possible.
For defecation, the first option is the only realistic one. Fortunately, continued successful execution of that prevents me from needing a colostomy bag.
How do you sleep in a bed?
I don’t often sleep well. One option is sleeping in
my non-standing wheelchair, but it leaves me stiff and achy. I really can't do it
for more than 2 nights consecutively due to comfort and edema issues.
The bed is preferable. At first, my husband used to lift me into it,
after having set up an array of pillows to give me a 30-45 degree
angle. He also propped additional pillows under my head and a pillow
under each of my hips to relieve pressure points. This lasted only a
short while, so I woke my husband anywhere from 3 to two dozen times
a night to adjust me. Now I still at times awaken him, and he
rotates my hips, straightens my legs, props my legs on a bolster
pillow towards the foot of the bed, varies the number of covers on
me, shifts other various body parts like my head or elbows, moves
propped pillows under me, adjusts me by pulling a bed mat on which I
lay, places
the urinal against me, and suctions mucous from my lungs.
For some years some of these problems had been alleviated by
my using a
Völkner Turning
System air mattress which rotates me throughout the
night without any extra propping. It reduced the chance of
pressure points, meaning I woke my husband far less as I stay much
more comfortable. It's trickier getting a urinal under me, and I
urinate more often in the middle of the night (because my fluids are
getting shifted more than at any other time); it sometimes also
moves my head, arms, or legs out of position requiring them to be
adjusted, but the positives far outweigh the negatives. With the
Völkner mat that gentle rotates me automatically all night (provided
the electricity is on), both of us got much more rest.
I also used to use an oxygen concentrator that takes
oxygen from room air and feeds it into the vent to make sure I
oxygenate well at night.
Before the vent, I slept mostly on each side. Each
morning while still in bed, I would be rolled into a face-down
position with the lower leg (below the knee) hanging off the bed
unsupported. Then ankle weights would be strapped on to stretch
tendons behind my knees. None of that is possible with using the vent.
How does a shower work for you?
It doesn't, anymore. I became too weak to be able to breathe that long in a steamy environment. Now, I have the lift installed that can take me to the bathtub, where the vent can hang off to the side in a way that works without undue stress on my stoma.
But when I used to take these, I used our walk-in shower with a ledge on which to sit. I'd park in our bathroom close to the shower door, which opens out. My husband lifted me a little higher than normal and stepped up and into the shower stall with me; then he sat me down on the ledge. During this process he wore special surf shoes with an incredible grip on them, and we put a mat down on the floor of the shower to help prevent slips as well. I sat on a towel folded twice for padding so the ledge is less painful on the bonier portions of my derriere. We kept the shower door slightly ajar because of problems breathing in the shower -- my sauna days are over. To prevent water from entering my stoma, the hole in my neck where the trach tube is inserted and to which the vent tubing connects, we must seal the trach well. We have a handheld showerhead that assisted with this process. My husband soaped me down from the top of my head to my toes (webmaster's note: I didn't mind this part at all). When this process concluded, my husband wrapped a towel around me to enhance the grip he needed to transfer me back into the power chair. Most days I didn't take a shower, or bath now; instead I am bathed in my wheelchair with a washcloth and water from a sink.
More about Deshae
Frequently asked questions: mobility issues
Frequently asked questions: pulmonary issues
Frequently asked questions: personal care issues
Frequently asked questions: her spirituality
Frequently asked questions: her tastes
Ulina (off-site)
Photo gallery (off-site)
Earliest years photos (off-site)
Port access photos (off-site)