Deshae Lott
determined sojourner
FAQ: Pulmonary issues
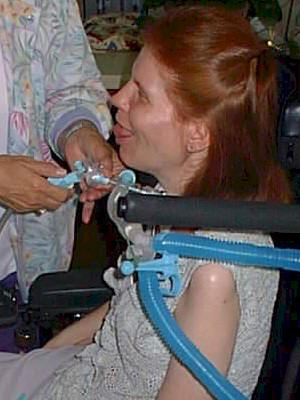
What does the suctioning process involve?
The vent tubing or circuits
connect to the trach tube in my neck via a part called a Ballard
catheter. This catheter
is another kind of tube that fits inside my trach tube and slides
down through it into my lungs.
Here are the steps:
- Attach a 5cc cartridge of
sterile saline water to an opening (the saline run) on the
Ballard.
- Squeeze the saline “bullet”
and shoot 2.5cc down into my lungs.
- Snake the catheter tubing
down into the top of my lungs.
- Turn on a pressurized
canister that sucks or vacuums out saline, mucous, air, etc. at
around 500 mm/Hg.
- Withdraw the catheter.
(Hopefully no part of my lung tissue will be traumatized;
this happens with too frequent suctioning or when the catheter
is lowered too far down.)
- Repeat process with the
remainder of the saline.
- Repeat process with no
saline (the “dry run”).
If mucous gets stuck in your tube, what do you do?
The tube must be pulled out by a skilled person and a new one slid in. It is not a pleasant experience, and sometimes it's needed as often as daily. Typically I change the tube once a month. But sometimes it's much more often. This is unpredictable, too, because it depends upon when the tube grows occluded by mucous.
Besides all of that saline, what other medications are you taking frequently if not regularly?
Xopenex, ipatropium bromide, and Mucamyst I inhale multiple times daily via a nebulizer machine attached to my vent’s circuitry/tubing; this lengthy process (in combination with the use of the Chest Vest for CPT and the Cough Assist device) requires help from skilled persons. I also take various anti-allergy medicines in pill and nasal form (Allegra or Claritin, Singulair, Flonase), the expectorant Mucinex, and Glycolax and Bisacodyl to compensate for weak abdominal muscles. From time to time other things get added -- some of those antibiotics being Nafcillan and Maxipime via IV infusion, Levaquin, Bactrum, Cipro, Tobrymycin, Fortaz, Keflex, Dicloxacill, Tequin, Factive, Augmentin, and others orally to fight off lung infections, Nystatin and Diflucan to fight off fungal infections when on those other antibiotics, diuretics to fend off edema, ibuprofen and acetomenephine to reduce fevers and aches, and pseudephrine to ease cold symptoms. I also take multivitamins and an iron supplement Niferex. To regulate my blood chemistry, I've also required transfusions as well as infusions of sodium, magnesium, manganese, and iron; sometimes I must have many months of venofer (iron by IV infusion plus Procrit shots). Drinking of hydrating fluids is essential on top of all of this (to keep my body freer of infection and my mucous thinner).
Is there more stuff you have to do, taking up even more time?
Yes. I nebulize almost always four times a day, during which my trach tube’s cuff is inflated, so I can't speak or do much during that process. Someone must be on hand to set this up and to watch in case something goes wrong, for I am unable to speak/voice a problem although I certainly can feel them! Twice a day after nebulizing I wear a Chest Vest which beats on my rib cage for 20 minutes at two different speeds, attempting to shake loose and break apart deposits in my lungs so they can be suctioned out. After this I get hooked to a Cough-Assist device that vacuums up phlegm for six cycles lasting about a half-minute combined; I repeat this process prior to being transferred to my bed for potential sleep, though that often proves compromised by coughing induced from pulmonary drainage when my body position shifts. This pulmonary health therapy process proves relentless in its necessity and time-consuming; however, since adding these elements to my pulmonary therapy routine, my difficulties with pneumonia in incidence and especially in severity have decreased substantially.
I also undergo stretching or range-of-motion therapy
occupying up to an hour a day, usually at least thrice a day.
Additional therapies include inhalation of various antibiotics, IV infusion, and designated postural drainage (essentially, lying on my back with my legs elevated so the lower lobes of my lungs drain; this is more intense than simply occupying a supine position in bed).
Then it takes a couple of hours extra every day for a caregiver to get me washed, dressed, and undressed; if a shower is included, that's another hour right there. With slower toileting routines and lots of time devoted to the business end of my health care, doing the basics for staying alive have become a full-time job; in fact, I spend more than 40 hours a week just on these tasks; often, far, far more than 40 hours a week. Crises like vent failures, visits from RTs, nurses, and doctors, x-rays, sputum samples, bloodwork tests, port-a-cath flushes, equipment checks and maintenance and replacement -- all of these aspects occupy my daily life. My survival requires a on-going "on-call" mode from me and my skilled caregivers as well as dedication to all of the many therapies necessary to prevent additional or greater crises.
More about Deshae
Frequently asked questions: mobility issues
Frequently asked questions: pulmonary issues
Frequently asked questions: personal care issues
Frequently asked questions: her spirituality
Frequently asked questions: her tastes
Ulina (off-site)
Photo gallery (off-site)
Earliest years photos (off-site)
Port access photos (off-site)